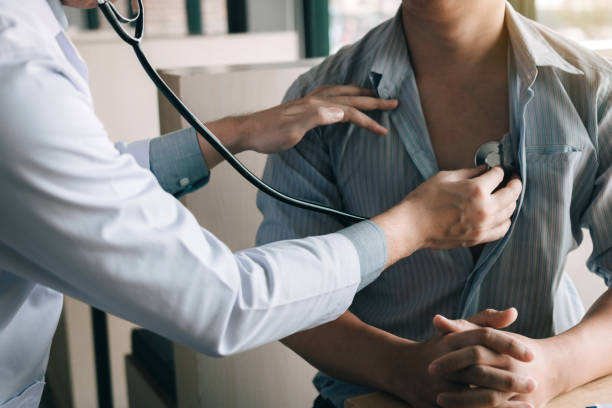
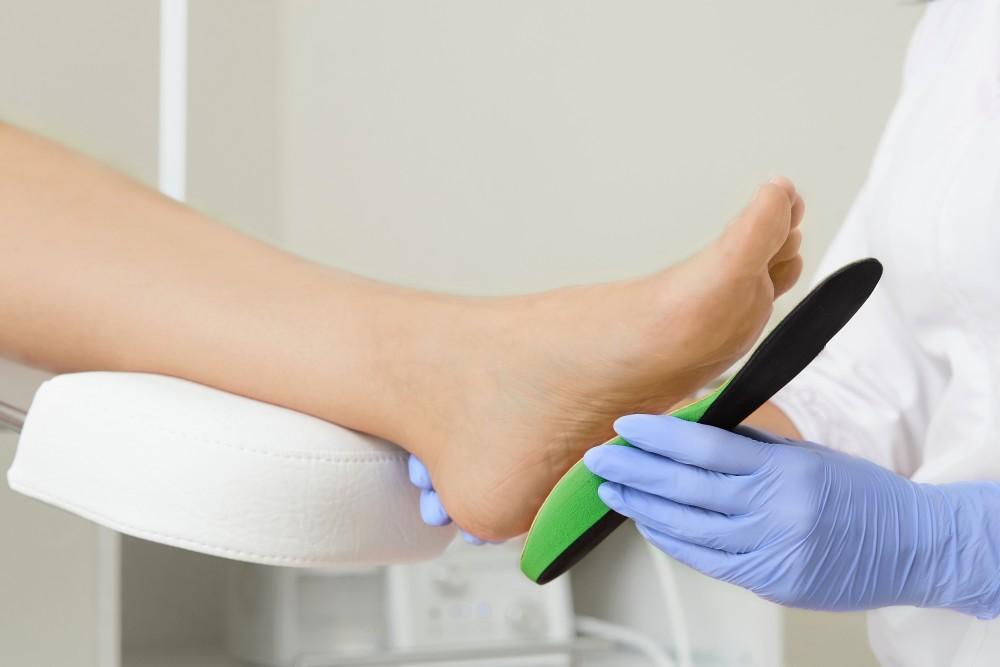
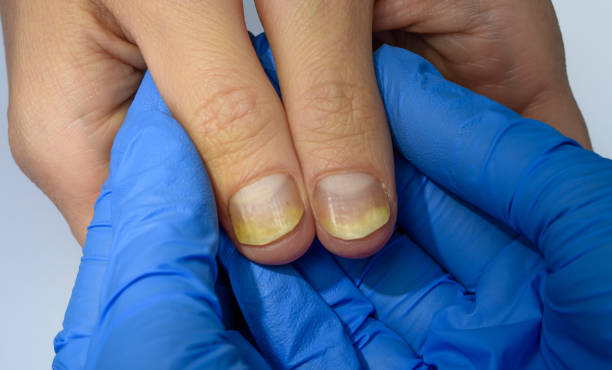
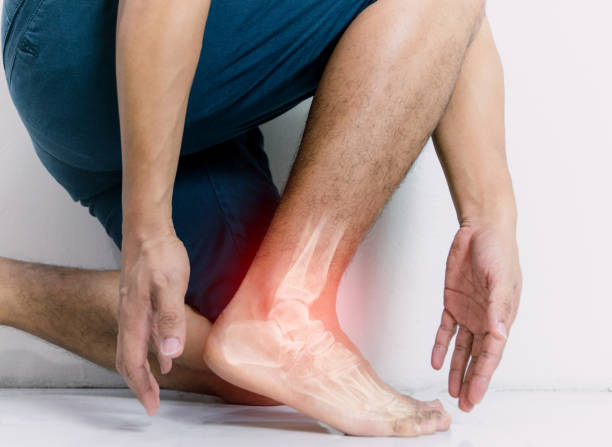
Our feet and ankles work hard and it is easy to take them for granted until a condition or injury arises. Surgery may be needed to repair severe injuries, improve function and reduce pain.
Podiatrist in Caloundra offer a range of surgical solutions that repair tissue and bone, and relieve pain. If you are considering surgery, it is important to understand the process.
Metatarsal Surgery
The surgery aims to reduce pain and deformity, distribute pressure more evenly throughout the ball of your foot, reduce callus/corn formation and improve toe alignment where possible. Lesser metatarsal surgery is commonly performed to treat hammer, claw and adductovarus (a condition where your toes curl under the ball of your foot). These conditions can develop due to muscle imbalance, ill-fitting shoes and arthritic changes.
During this procedure, your doctor will insert a pin, screw or plate to keep the bone in place while the injury heals. This is often recommended for zone 2 Jones fractures as well as chronic injuries where conservative treatment has failed.
Dr. Peter Shelton BSc Hons utilizes a minimally invasive ambulatory surgical technique that involves an extremely small incision on the top of your foot. This allows for an optimal cosmetic result and also reduces swelling, pain and recovery time.
After your doctor, has closed the incision, you will be able to begin walking on the injured foot with a special post-op shoe or boot. You may need to use crutches for a short while as you heal. As you continue to heal, your doctor will gradually increase your activity level. This will ensure that your bones heal correctly, without re-injuring the area. When your injury has fully healed, you will be able to wear regular shoes again.
Morton’s Neuroma Surgery
Morton’s neuroma is pain and numbness caused by compression of a nerve between two metatarsal bones at the ball of your foot. The cause is not fully understood, but tight shoes and repetitive squeezing can cause the nerve to become thickened and produce a nodule (neuroma). Non-surgical treatment of this condition is often effective with shoe modification, insoles, calf stretchers, pain killers and occasionally cortisone injection.
If non-surgical treatment fails then a surgical procedure called neurectomy can be performed. Your surgeon can either remove the swollen part of the nerve or release pressure on the affected area. Depending on the surgeon’s preference this is done via an incision on the top or bottom of your foot. 85% of patients treated with neurectomy report good or excellent results, although multiple neuromas in one foot tend to have worse outcomes.
After this surgery your foot will be swollen, which is a normal response to any operation. Keeping your foot elevated as much as possible, and not walking on it for the first week will help reduce this swelling. The wounds usually heal well, but occasionally infections occur, which can be treated with a course of antibiotics. A small number of people may develop permanent numbness as a result of this surgery. This is a very rare occurrence. Usually the numbness is reduced over time, but this can take up to 6-9 months to disappear completely.
Arthroplasty
Arthroplasty is a surgical procedure that replaces some or all of a joint. Your healthcare provider removes the damaged part of the joint and replaces it with an artificial part, called a prosthesis. The artificial part is usually made of metal, a type of plastic or ceramic.
Your doctor may recommend this surgery if nonsurgical treatments such as medications, physical therapy, and activity modification don’t help. The benefits of arthroplasty include less pain and stiffness, more mobility, and a better quality of life.
Before arthroplasty, your doctor will ask about your health history and perform tests to check for conditions that may affect your recovery. These may include blood work, an electrocardiogram and a chest X-ray. You may also need a CT scan or an MRI to plan your surgery.
On the day of your surgery, you will receive general or local anesthesia to numb your body. Then, your surgeon will make an incision over the knee area. They will remove the diseased or damaged bone and cartilage. They will implant the replacement parts into your thighbone, shinbone and kneecap.
Then, they will close the incision with stitches or surgical staples and apply a dressing. After the surgery, you will rest in the recovery area until your blood pressure, pulse and breathing are stable. You may stay in the hospital for several days.
Osteotomy
Osteotomy is a surgical procedure that involves breaking or adding bone to change the alignment of a joint. This can help relieve pain and stiffness caused by conditions like arthritis. It can also improve alignment and function. It is sometimes combined with other procedures to help repair damaged tissue.
For this type of surgery, you’ll be under general anesthesia. Your surgeon will make an incision over the area of your bone that needs to be changed. Then, using a surgical saw, he or she will remove a section of your bone. Your doctor may use other tools to help remodel the shape of your bone, such as hammers or chisels. Your doctor will then fill the new space with graft material or put in a metal plate to hold your bones together until they heal.
A calcaneal osteotomy is usually done to treat a condition called Morton’s neuroma, which is caused by impingement of nerve branches in the heel bone (heelbone). It can also correct problems such as flatfoot deformity and arthritis.
For this surgery, Coastal Podiatry at ( https://www.coastalpodiatry.com.au/ ) will make an incision on the outside of your knee. Then he or she will cut your tibia (shin bone) or, in some cases, your femur (thigh bone). The location of the cuts and the way they are made will determine the type of osteotomy you have. Tiny screws and a metal plate are used to hold the bones in place while they heal.